
March 6, 2023
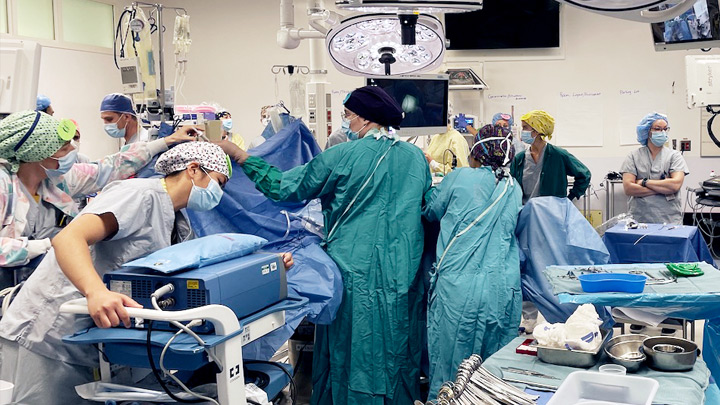
An EXIT Procedure Simulation gets underway in an operating room at the Foothills Medical Centre. Photo courtesy of eSIM Provincial Simulation team.
Story by Mirette Dubé, Sue Barnes, Julia Haber & Nancy Soliman
CALGARY — High-risk operations in a surgical suite call for extreme preparation and organization of every member of the medical team. However, some procedures are so rare that teams need the opportunity to practise and perform the surgery in advance to ensure the best processes and systems are in place when the real thing happens.
This is where simulation exercises have a huge role to play.
In November 2022, teams from the Foothills Medical Centre, Alberta Children’s Hospital and the Educate, Simulate, Innovate and Motivate (eSIM) Provincial Simulation Program, planned and simulated a high-risk special delivery — an Ex-Utero Intrapartum Treatment (EXIT) procedure — using special medical mannequins of a mother and newborn.
This is a special delivery procedure performed when it’s anticipated that a baby will face an immediate, critical problem once separated from the mother at delivery.
In the case of airway obstruction, for example, an EXIT procedure gives the surgeon time to clear the baby’s airway, secure a breathing tube, and provide adequate ventilation, before the baby is separated from the mother. Once the baby is stable enough for delivery, the umbilical cord is cut, and the newborn is transferred to the care of the neonatologist and the pediatric surgeon.
“As you can imagine, such an endeavour involves bringing together a huge number of people, from different healthcare backgrounds, to perform a rare and high-stakes set of steps,” says Dr. Julia Haber, anesthesiologist for the simulation preparation and faculty.
With seven teams involved — including Obstetrics, Maternal Fetal Medicine, Neonatology, Maternal and Pediatric Anesthesia, the Perioperative team, Pediatric Otolaryngology and, of course, the patient and family — smooth coordination is vital. Ensuring everyone is well-rehearsed, comfortable and the environment that surrounds the teams is tailored for the workflows that follow, is key to safe, efficient and quality care.
“Every team had the opportunity to voice concerns and suggestions during the debrief which made the day of the procedure run very smoothly,” says Dr. Nancy Soliman, perinatologist and obstetrician for the actual patient. “All equipment was identified and set up well ahead of time, and all potential kinks in the process were identified through the simulation.
The simulation and debriefing identified multiple improvements, including operating room layout, team communication, how to solidify team roles and responsibilities, equipment, IT process improvements and care of the family members as well as post-delivery care.
“The conversations that occurred to clarify clinical steps and transitions of care between teams would not have occurred at all prior to the actual simulation event. These conversations would not have been possible during an actual EXIT procedure,” adds Dr. Haber.
The eSIM team serve as quality-improvement and patient-safety thought leaders for AHS. They have developed internationally recognized approaches for these types of systems simulations where the focus is not only on medical team training, but also takes a broader look to identify any potential gaps within the healthcare system, environment, technology, process or procedures.
“Right from the engagement of the simulation team, they were responsive, knowledgeable and collaborative,” says Dr. Soliman. “They recreated the model that we needed to work with. During the simulation, they ensured all necessary equipment was set up ahead of time and kept the group on task.”
The provincial eSIM team is a provincial program dedicated to improving frontline care through education, systems testing and working with a broad range of teams. eSIM has more than 16,000 participants and more than 2,000 sessions per year across all zones in Alberta. For more information, email the eSIM team at esim@ahs.ca.