
April 18, 2023
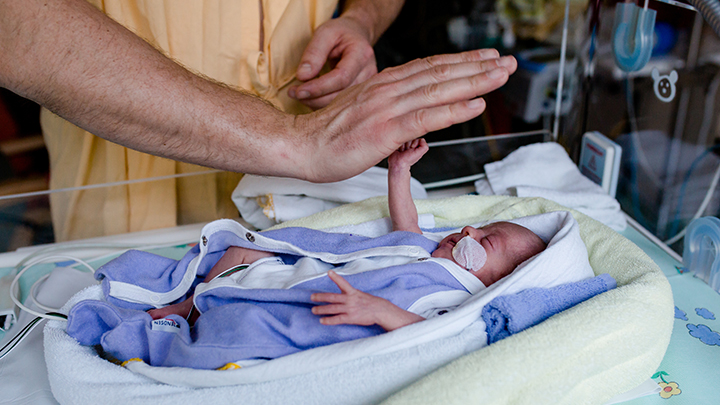
Fewer critically ill newborns are requiring emergency department (ED) visits and hospital readmission, thanks to the introduction of the Alberta Family Integrated Care (FICare) model in Neonatal Intensive Care Units (NICUs) across Alberta. FICare encourages parents to actively participate in their baby’s care and work alongside their NICU healthcare team to build the knowledge, skills and confidence needed to parent their babies in both the NICU and at home.
Story by Vanessa Gomez
CALGARY — Fewer critically ill newborns are requiring emergency department (ED) visits and hospital readmission within seven days after going home thanks to a new model of care in all 14 neonatal intensive care units (NICU) across the province.
Alberta Family Integrated Care (FICare) encourages parents to actively participate in their baby’s care and work alongside their NICU healthcare team to build the knowledge, skills and confidence needed to parent their babies in the NICU and at home.
Following the provincewide introduction of Alberta FICare in 2019, ED visits have dropped 26 per cent, and hospital readmissions are down 37 per cent, for former NICU patients in the first week after leaving hospital. The average length of stay in the NICU has also been reduced by half a day, allowing babies to go home sooner. FICare is helping to improve patient flow through sites and programs, one of four key priorities of Alberta Health Services (AHS).
“Having a baby in the NICU can be a stressful experience for parents and learning to care for a preterm baby both in the hospital and at home requires extensive support over time during the hospitalization,” says Dr. Deborah McNeil, scientific director of AHS’ Maternal, Newborn, Child and Youth Strategic Clinical Network, which was involved in the development of FICare.
“Nurses have moved into an educational role and support parents who want to be part of their baby’s NICU journey when they are ready.”
Parents in the NICU are supported and educated to provide skin-to-skin care, change diapers and clothes, participate in bedside rounds, bath, weigh, feed, take temperatures, and provide comfort during treatments and procedures.
“We’ve always had excellent care in the NICUs, but this model enables healthcare teams to integrate families within the healthcare team,” says Dr. McNeil, adding early involvement of parents in care has many benefits for preterm babies, including healthy brain development, less feeding and breathing supports, and stabilized breathing and heart rate.
Approximately 50,000 babies were born in Alberta in 2021, with 8.8 per cent of them — about 4,400 — born preterm and requiring care in a NICU. A stay in the NICU can range from two to nearly 100 days.
Kyrsten Franz’s son Theodore was born at 27 weeks in early November and received care at the Rockyview General Hospital NICU.
“If family integrated care didn’t exist, this experience would be 10 times harder,” says Franz. “Being able to care for my baby in the NICU helps normalize the experience. I can still make decisions and do something as simple as diaper changes, and we are constantly reminded that we’re an important part of our child’s care.”
As part of FICare, parents receive a journal that contains resources and information, outlines how parents can participate in bedside rounds, and provides space for parents to write about their baby, their NICU journey and things they’ve learned, and to record their questions.
“It’s overwhelming to be introduced to a large multidisciplinary team,” says Karen Benzies, professor with the Faculty of Nursing, and Adjunct Research Professor with the Departments of Pediatrics and Community Health Sciences, at the University of Calgary. “Parents play an integral role in the care of their baby; it’s important they have a voice in their care and that the teams value and respect their unique knowledge about their baby.”
It’s estimated the reductions in the NICU length of stay have saved the health system about $1.2 million over a two-year period.
Expansion of FICare across the province was made possible through partnerships between the Maternal, Newborn Child and Youth SCN and the University of Calgary, and funding from Alberta Innovates (Partnership for Research and Innovation in the Health System), the Alberta Children’s Hospital Research Institute, the Canadian Institute of Health Research and Alberta Health/Alberta Health Services Health Innovation Implementation and Spread Fund.