
January 22, 2014
Story and Photo by Colin Zak
Alex Petric’s life changed forever last March.
The 29-year-old fractured his spinal cord in a diving accident while on vacation in Panama.
“I dove into the water and hit a sandbar. I was paralyzed immediately from the waist down,” says Petric, who previously worked as a paramedic in Winnipeg. “I tried everything when it comes to treatments. I even went to California to get some intensive rehabilitation.”
However, a new study transplanting neural stem cells into patients with spinal cord injuries could offer hope to Petric and patients like him.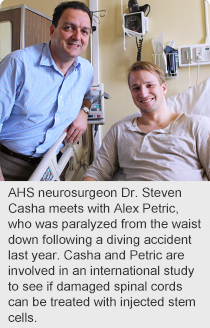
The study looks at whether it is safe to inject stem cells into patients’ spinal cords, and could lead to more studies as to whether the treatment could help improve sensory and motor function in patients.
Petric was the first patient in North America to participate in the study and underwent the procedure this month at Foothills Medical Centre.
“I had everything to gain and nothing to lose,” he says.
The procedure uses neural stem cells – cells that are committed to becoming neural tissue – that are derived from donated fetal brain tissue. The brain cells are harvested, grown, frozen and prepared for injection by the U.S. firm Stemcell Inc.
“The aim of stem cells, and other technologies like it, is regeneration. Patients with spinal cord injuries have lost part of their spinal cord and some of the supporting structures that allow it to function. Regenerative strategies want to replace what’s been lost, in term of neurons or nerve cells and supporting cells, and provide healthy cells to support those which have survived,” says Dr. Steven Casha, an Alberta Health Services neurosurgeon and assistant professor at the University of Calgary, who is leading the study in Calgary.
“Patients are very excited about stem cells because it is possible, theoretically at least, to completely restore a normal spinal cord. However, the technology is still in its early stages.”
Most patients with spinal cord injuries would have had their spinal cord exposed at the time of their injury, explains Casha. The procedure involves re-exposing the spinal cord, determining the location of the injury, and making four injections of stem cells: two injections approximately a centimetre above the injury, and two a centimetre below.
Seven patients have already undergone the procedure in Switzerland.
“What we know so far is that two of the first three patients had an improvement in sensory function,” Casha says. “It’s encouraging. This is something to build on.”
However, Casha says the benefit of the procedure for patients remains unknown.
He says the injections probably provide new nerve cells and large insulating cells around the existing nerves, but this does not guarantee that those will make functional connections with a patient’s existing spinal cord.
While there are many surgical and rehabilitation options to treat patients who have spinal fractures, there are relatively few treatment options for spinal cord injuries, which result in loss of neurological function.
“There has been talk about stem cells for years and years; it’s captured the imagination of a lot of people, especially patients,” Casha says. “It’s exciting to see it finally coming to fruition.”
The study is currently recruiting a dozen patients with injuries to the thoracic spinal cord. Since the study is a Phase 1 clinical trial, it is focused on safety rather than actual benefit of the treatment. As a result, there are strict selection criteria for participants.
“As the technology moves forward, there will be more patients who meet the criteria and can participate,” says Casha. “Because this is a Phase 1 trial, our hope is that there are no adverse effects for patients. Perhaps, if we’re lucky, we’ll see some improvement in motor function or sensory function.”
While Petric was pleased to participate in the research trial, he is cautiously optimistic.
“Hope is a good thing – it helps you hold on to what’s possible,” he says. “At the same time, I also need to accept the life I have now.”