Before Surgery | Pre-Admission Clinics | Day of Surgery | Discharge | At Home
Your child needs heart surgery. Now what? Coming to the Stollery Children’s Hospital for surgery is a big event for you, your child, and your family. Getting ready and thinking clearly can seem almost impossible at this time. Take the time to talk together before coming. Knowing what to expect and how to prepare ahead of time will help to decrease anxiety for both you and your child.
If your child is coming to the Stollery for any other surgery, visit Your Child’s General Surgery, Surgery and Operative Services.
While you wait for your child’s heart surgery date, there are some important things to do to prepare and information you will need to know.
To help prevent infection after heart surgery, babies and children with teeth must see their dentist before heart surgery. All required dental work needs to be complete before they come. We will give you a form to take to your dentist. Have them fill it out, and ask them to fax it to our case coordinator at 780-407-3598. Bring a copy with you to your child’s pre-operative appointment at the Pre-Admission Clinics.
Some children may need antibiotics before dental cleanings and treatments. Check with your child’s cardiologist if you are unsure whether or not antibiotics are required.
If your child has already seen the dentist recently (within six months of your child’s surgery date), ask your dentist for a letter confirming that your child was seen and that all the required dental work was completed. Have them fax this to the case coordinator at 780-407-3598.
If your child is ill before or on the day of surgery, your child’s surgery may be postponed. Contact the surgical case coordinator by calling 780-407-7709 for any of the following reasons:
Children can continue to take most medications until the day of their surgery. Sometimes, certain medications (especially blood thinners including aspirin) need to be stopped several days before surgery. If you are unsure of what medications to stop, call your surgical case coordinator or cardiologist to confirm.
For your child’s safety, it is important that the bedside space is clean and clear of clutter. If you plan to stay at the hospital with your child, bring only what is really needed. This ensures that the staff has quick and easy access to your child at all times.
The Pre-Admission Clinics (PAC) is an outpatient clinic that prepares children and their parents for surgery.
The Surgical Case Coordinator will phone you with the date and time of your PAC appointment. Typically, this appointment is a day or two before surgery and the arrival time is usually 7:00 am.
Some of the people you will meet*:
You may also meet:
Other healthcare team members may be consulted to ensure the complete care of your child while in hospital.
Some tests your child will have*:
*We are unable to schedule definite times for any of the persons or tests above because all are based on availability of the team members. We will make every effort to have your day completed in a timely manner.
You will be offered a tour of the Pediatric Cardiac Intensive Care Unit (PCICU) and/or the Cardiology Inpatient Unit (4C) depending on the type of heart surgery your child is having. This is where your child will be transferred after finishing in the OR. This tour is optional, but it is highly recommended if this is your child’s first heart surgery.
Some things you could ask:
We encourage you to write your questions down in advance and bring them with you.
The pre-admission clinic nurses will contact you the afternoon before surgery to tell you:
NPO means nothing by mouth. All children, even babies, need to have an empty stomach before going for surgery. This includes stopping tube feeds.
Children are usually admitted to the hospital on the day of surgery. You may be asked to register with the Admitting Department, or to go to 1C3 Pre-Admission Clinics (PAC) directly. Admitting is located on the main floor of the hospital, behind the glass elevators.
After registering with admitting, you will return to the pre-admission clinic where you were on the day of your PAC visit. The nurses there will get your child ready for surgery.
Your child will:
Ask your anesthesiologist during your PAC visit if you can go with your child as they are transported to the OR. Sometimes, one parent or guardian is allowed. If you go, you will be asked to wear a hat over your hair and a gown over your clothes to prevent outside germs from coming into the clean environment of the operating room.
Once your child arrives to the OR:
Your child could be in the operating room for an hour or more just getting prepared before the actual operation begins. After your child is comfortably sleeping under the supervision of the anesthesiologist, the team will continue to prepare your child. They will use many types of equipment to monitor and support your child during surgery. Some of these will still be in place after the surgery is over and when your child leaves the OR.
Waiting while your child is in the OR
While your child is having their surgery, you will be holding all of your child’s and your own personal belongings. On the day of surgery, bring only what you and your child need for the first 24 hours, and only what you can carry. You can bring the rest once settled in your room after surgery.
Your PAC nurse or surgeon will tell you how long the surgery might take. The length of time that a child will be in the OR is sometimes difficult to estimate. The teams in PAC and the OR will make sure that you know the plan for receiving updates while your child is in the OR. When the surgery is done, the surgeon will come and meet with you at a designated location to discuss how the surgery went and how your child is doing. Before leaving PAC, make sure your cell phone number is up-to-date in your child’s chart.
Once the surgery is complete, your child will be transferred from the operating room to one of the following two units:
The Pediatric Cardiac Intensive Care Unit (PCICU) on the 6th floor of the Mazankowski Alberta Heart Institute (Maz)
The 4C Cardiac Inpatient Unit on the 4th floor of the University of Alberta Hospital (UAH)
Daily Bedside Rounds
Parents are encouraged to be present for, and to participate in, daily rounds with the healthcare team. This is where the team meets to discuss your child’s medical status and clinical plan. You will learn more about how your child is doing as well as any tests, treatments, or procedures that may be needed. After the team is done, you are encouraged to ask questions. These rounds take place at your child’s bedside and typically start around 8:00 a.m. Some days, it may take most of the morning for the team to make their way around the unit as they visit each patient.
Breast Feeding Moms
There are breast pumps available for your use. Sterilization bags and one set of attachments will be provided to you for the length of your baby’s hospitalization. Labels and bottles will also be provided. Unlabeled breast milk will be disposed of. There are freezers where your milk can be stored. Talk to your bedside nurse for more information on how to locate these freezers and supplies.
Readiness for discharge is not determined by time, but by meeting a set of required criteria. Some children may take only a few days to meet discharge criteria. Others may require a week or more. Once your child meets the criteria specific to their age and condition, discharge from hospital can be considered.
Most children can go directly home after discharge from hospital. If you have come from another city, your child may be transferred back to the hospital nearest your home. In some cases, patients are required to stay in Edmonton after discharge until they have completed their post-operative clinic visit and the cardiologist feels it is safe to return home. Do not hesitate to ask your doctor or nurse if you have questions or concerns.
When you leave the hospital, you will receive an information sheet that tells you about your child’s care at home. You will also be given a copy of the medical discharge report and the unit discharge instructions. Bring these information sheets with you when you return to the Stollery for follow up at the 4C2 Cardiology Outpatient Clinic, or when see your own doctor next.
Most children increase their activity at their own pace. Teenagers may need reminders not to overexert themselves in the first few weeks. Let your child set the pace. Don’t lift infants or small children under their arms. Avoid rough play and contact sports. Insist on rest periods. Avoid front seats with airbags. Car seats and seat belts should be used properly at all times. Children are generally ready to return to school or day care within one to two weeks after surgery.
Changes in behaviour are a normal part of recovering after heart surgery. A child’s surgery is a difficult experience for everyone in the family, and behaviour changes are just one of the ways children communicate. You may notice for a while after surgery that your child might cry more, act out in anger, need more attention, or have changes in appetite or sleep routines. These changes are not uncommon. Your presence, patience, and understanding will help to reassure your child that they are safe and well. Your child’s normal personality will come back again, usually within the first few weeks.
It may take time for your child’s appetite to return to normal. Don’t force your child to eat, but do encourage fluids to keep them well hydrated. Eventually, as they begin to tolerate more and their appetite returns, encourage them to eat a healthy diet to promote healing and recovery. If your child has special dietary needs, your dietitian will provide teaching and resources in hospital to ensure you feel comfortable returning home.
After heart surgery, children require an echocardiogram (ultrasound of the heart). This is done at least once before they go home, and again around 10 days after surgery. If your child is still in hospital 10 days after surgery, both echocardiograms will be done before you leave. If you have been discharged before day 10 after surgery, an appointment will be made for you to have this echocardiogram done in your local outpatient cardiology clinic.
Children usually require medicine for a while after they go home. You will be given a list of medications that have been ordered, and the necessary prescriptions, before you leave the hospital. Be sure to understand what medicine your child is taking and why. If you have questions, talk to your doctor, nurse, or pharmacist. Call your family doctor or cardiologist for refills before you run out of medication.
Emergent Concerns
If you have an emergent concern about your child, call 911 to access emergency services immediately. Some examples of emergent concerns are trouble breathing, seizures, fainting, or not waking up.
Urgent Concerns
If you have any questions or concerns within the first six weeks after your child leaves hospital, and you think they are related to your child’s heart, contact your closest pediatric cardiology clinic during regular business hours. If you need to speak with a physician outside of business hours, call your hospital switchboard and ask to speak with the pediatric cardiologist on call. Examples of urgent concerns include changes in feeding, changes in breathing, extreme or prolonged changes in behaviour, changes in colour, signs of infection, or signs of water retention.
Ordinary Health Concerns
If you have questions or concerns about your child’s general health, contact your child’s pediatrician or family doctor. Examples of general health concerns include cough or cold symptoms, rashes, questions about routine immunizations, injuries from ordinary activities.
Surgery & Operative Services Program
MyHealth.Alberta.ca
Your Child's Surgery
Jump to:
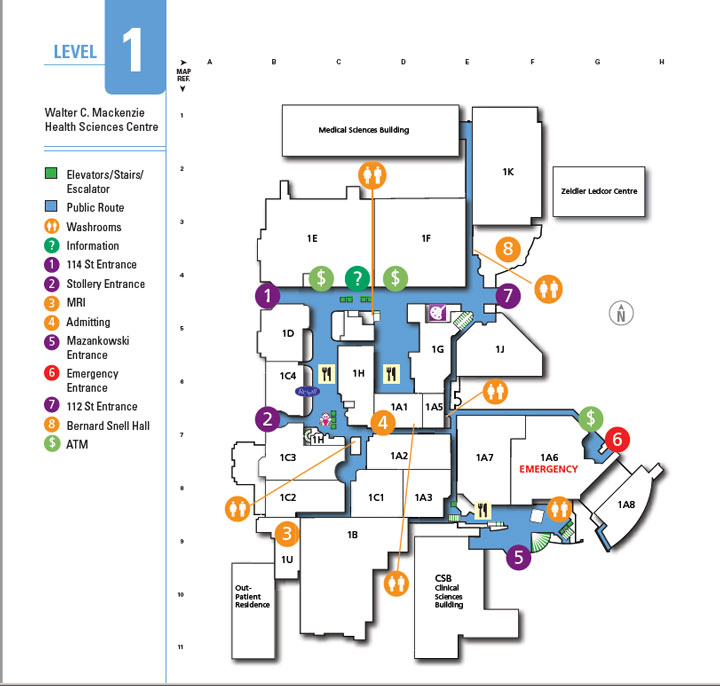
1st Floor
Includes Pre-Admission Clinics
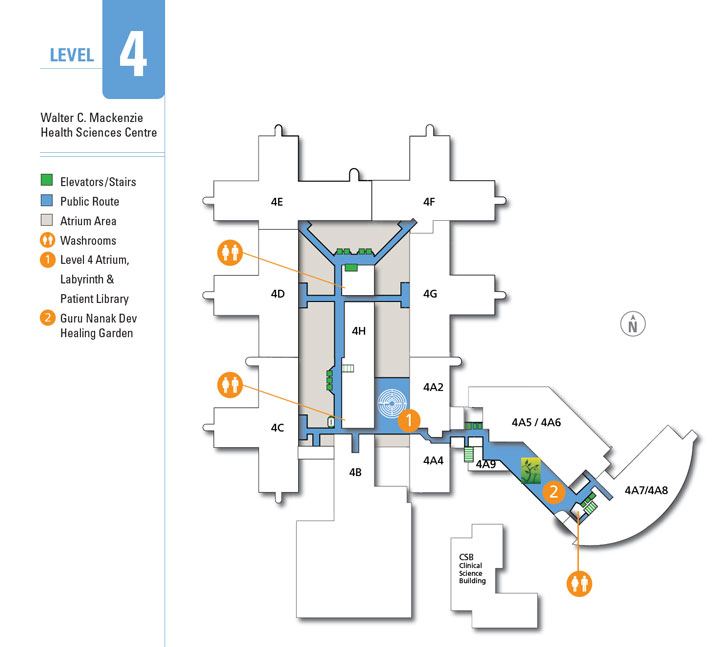
4th Floor
Includes Unit 4C